Resources
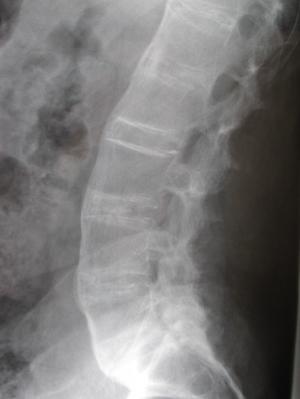
Ankylosing spondylitis is an inflammatory form of arthritis that affects the spine as well as peripheral joints such as the hips and shoulders.
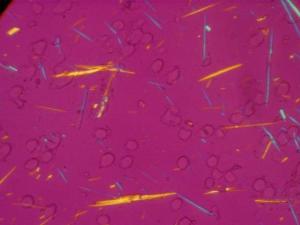
Gout is an extremely painful form of inflammatory arthritis, caused by an accumulation of uric acid crystals in the joints.
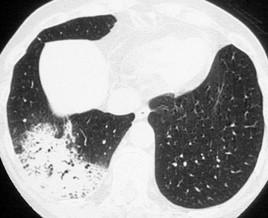
Interstitial lung diseases are conditions that result from inflammation and damage to the lungs that impairs the transfer of oxygen into the blood.
Psoriasis is an autoimmune disease (immune system attacks the patient) of the skin characterized by raised red areas of the skin called plaques.
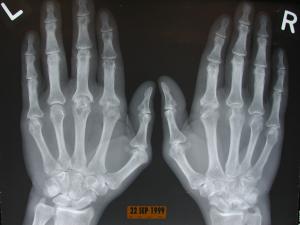
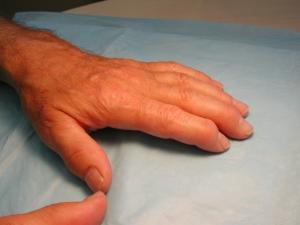
Rheumatoid arthritis (RA) is an autoimmune disorder in which an immune attack against the small joints of the hands and feet occurs due to abnormal targeting of this tissue by the immune system.
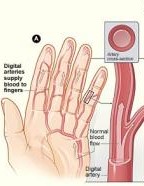
Scleroderma is an autoimmune disease characterized by an excess formation of fibrous tissue (scar tissue) in various organs including the skin, lungs, heart, intestines, that cause these organs to not work properly.
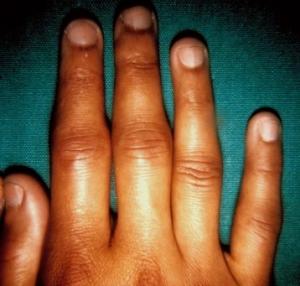
Systemic Lupus Erythematosus (SLE)
Systemic Lupus Erythematsus (SLE) is a chronic autoimmune disease that occurs when the body's immune system attacks its own tissues. Inflammation caused by SLE can affect joints, skin, kidneys, blood cells, brain, heart and lungs.